Perhaps the easiest way to understand blood sugar fluctuations is to examine what happens in our body under various physical loads.
In a resting state, the digestive tract breaks down complex carbohydrates from food into glucose. Simultaneously, the beta islet cells of the pancreas release insulin into the bloodstream. Insulin acts as a “key,” opening pores in cell membranes, allowing glucose to flow into cells as an energy source.
The alpha islet cells produce glucagon to ensure a constant energy supply, enabling the body to replenish glycogen stores in the liver and muscles. These stores are used during periods without food or when we suddenly need a large amount of sugar.
This process is called glycogenolysis, where, under the influence of stress hormones (adrenaline, cortisol), glucagon breaks down stored glycogen into glucose, which enters the bloodstream or directly fuels muscle metabolism.
During physical activity, blood sugar levels fluctuate depending on the type and intensity of the exercise.
A pleasant, non-strenuous activity, for example, can lead to a decrease in blood sugar. Since we’re not overly taxing ourselves, we don’t deviate significantly from the normal state, resulting in increased energy demand in the muscles, heightened insulin sensitivity, and increased glucose uptake.
However, during high-intensity exercises (like heavy weightlifting, sprints, or intense aerobic workouts), when we subject ourselves to significant stress, insulin production halts. The sharply increased energy demand is met through glycogenolysis, facilitated by stress hormones and glucagon. Adrenaline stimulates the liver to release glucose into the blood, raising blood sugar levels.
When we finish exercising and the stress ceases, regeneration processes begin. Insulin sensitivity increases again, the body starts utilizing consumed nutrients more effectively, and muscle and sugar stores are replenished.
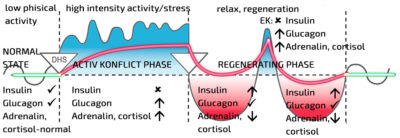
What Happens During Conflict Activity?
When we’re in a conflict situation, we’re under the same kind of stress as during intense exercise, potentially for weeks or months, as long as the conflict persists—even if this isn’t always visible externally. The difference is that the stress is not (only) physical but emotional, placing a much greater burden on the brain. In an active conflict state, stress hormone (adrenaline, cortisol) production doesn’t stop, even at night.
If the conflict triggers our resistance and demands that we fight, and we feel strong enough to shape the situation according to our intentions (i.e., we experience a “conflict of resistance”), the process mirrors intense exercise: insulin production is blocked, and glycogenolysis, driven by stress hormones and glucagon, increases blood sugar levels.




